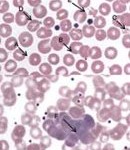
Posted July 11, 2012 Another interesting article on Bartonella. Often times the lyme symptoms aren’t just cause by the Borrelia burgdorferi there can be co-infections such as Bartonella. Good article
Bartonella: A New Frontier in Chronic Disease
New molecular test leads to surprising new research implicating Bartonella in rheumatological illness
By Edward B. Breitschwerdt DVM, CEO/CSO Galaxy Diagnostics & B. Robert Mozay
New research recently published in the journal of Emerging Infectious Disease supports an association between Bartonella infection and rheumatological symptoms. The researchers tested 296 immunocompetent patients for evidence of Bartonella infection. Bacteremia with one or more Bartonella species was found in (41 percent) of patients with a prior diagnosis of Lyme disease (47 percent), arthralgia/arthritis (21 percent), chronic fatigue (20 percent) and fibromyalgia (6 percent). This study follows two decades of medical case series research implicating Bartonella infection in chronic diseases affecting the joints, neurological and vascular systems.
Bartonella are highly fastidious, immune-evasive, gram-negative bacteria which infect at very low levels of detection. As a result, conventional serological and polymerase chain reaction (PCR) testing technologies are of limited value for the confirmation of infection. These surprising new findings were made possible by a new testing technology developed by researchers at the North Carolina State University College of Veterinary Medicine(NCSU-CVM). The NCSU research team discovered a way to overcome past testing challenges through the development and use of a propriety enrichment media (Bartonella alpha-proteobacteria growth medium or BAP-G-M). When paired with highly sensitive PCR testing, the BAPGM media increases the sensitivity of detection by 4 to 5 times over conventional methods.
 Popularly known as the key agents in cat scratch disease (CSD), trench fever, and carrion’s disease, Bartonella were essentially rediscovered in the 1990s with the emergence of HIV and the clinical application of DNA testing technologies. There are now over 25 characterized species of Bartonella, 12 of which have been documented as pathogenic for humans. A wide range of animals serve as natural hosts for this zoonotic bacteria, most significantly the cat and rodent populations, which may be transmitted by a number of different vectors including fleas, lice, ticks, and biting flies.
Popularly known as the key agents in cat scratch disease (CSD), trench fever, and carrion’s disease, Bartonella were essentially rediscovered in the 1990s with the emergence of HIV and the clinical application of DNA testing technologies. There are now over 25 characterized species of Bartonella, 12 of which have been documented as pathogenic for humans. A wide range of animals serve as natural hosts for this zoonotic bacteria, most significantly the cat and rodent populations, which may be transmitted by a number of different vectors including fleas, lice, ticks, and biting flies.
A 2004 Nature article describes Bartonella as one of the most important pathogens in emerging infectious disease along with Helicobacter pylori (H. pylori). Unlike H. pylori, however, Bartonella is not localized to the gastrointestinal (GI) tract, but can infect multiple systems in the body.
Well-established as life-threatening in patients with compromised immune systems, the emerging research indicates that Bartonella are also a problem in patients with competent immune systems. Research on HIV patients, suggests a pattern of progressive presentations of bartonellosis from mild CSD symptoms to peliosis hepatitis and bacillary angiomatosis. Bartonella has also been documented as a cause of culture-negative endocarditis, osteomyelitis, meningitis, encephalitis, neuroentinitis and vasculitis.
Mounting case evidence indicates that atypical presentations of cat scratch disease may not be nearly as uncommon as previously thought, especially in high-risk patient populations. Symptoms may range from recurring fever, headaches, insomnia, joint/muscle aches and pains to arthropathy, myalgia, neurocognitive and neuromotor dysfunction, seizures, vasculitis, and vaso-proliferative tumors or lesions, as well as the more common lymphadenopathy and splenomegaly.
Risk factors associated with Bartonella infection include high levels of animal contact and vector exposure. In an earlier study using the Bartonella ePCR™ test, the NCSU research team found that 23.9 percent of 192 patients with occupational animal contact or extensive arthropod exposure were bacteremic with one or more Bartonellaspecies when blood, serum and BAPGM enrichment culture PCR results were combined. Although this high prevalence of bacteremia is biased by testing at-risk, sick individuals, it clearly demonstrates that intravascular infection with Bartonella species is much more common in immunocompetent patients than was previously suspected.
Importantly, Bartonella infection may also represent a safety concern in the blood supply in transplant medicine and chronic disease management. Of particular concern are medical conditions managed with therapeutic regimens that cause immune suppression, including rheumatologic diseases such as rheumatoid arthritis or lupus, or organ transplantation. Other conditions, such as cancer, may involve the use of medications that cause immune suppression, such as high-dose steroid components of lymphoma protocols. Blood banking practice must also consider the potential for the transmission of Bartonella through transfusion of blood products. These safety issues indicate the need for better prevalence studies to determine the cost-benefit of screening for safety reasons, including the screening of blood products.
Recommendations for medical practitioners:
- Consider testing patients at high risk who present with general rheumatic or neurological symptoms for Bartonella infection.
- Make clinical protocols involving immune suppression, including transplantation and cancer treatments, safer by testing high-risk patients for Bartonella infection.
- Advise patients to exercise routine precautions to avoid animal bites and scratches when dealing with domestic or wild animals and to avoid exposure to arthropod and insect vectors.
The emerging research on Bartonella is very compelling and the need for clinical research that directly addresses the role these bacteria play in human and animal health is clear. Because the genus Bartonella involves multiple animal reservoirs, animal and human disease, arthropod and insect vector transmission, and an environmental impact on human health, multidisciplinary research efforts following the One Health Initiative are needed to effectively address the far-reaching implications and the redefinition of “bartonellosis” as an emerging infectious disease of the 21st century.